Rethinking Metabolic Safety: The Hypothalamus as a Critical Target for Preventing Antipsychotic-Induced Weight Gain
December 23, 2025
October 15, 2025
Obesity remains a major global health challenge driven by imbalances in energy intake and expenditure, yet traditional calorie-centric models cannot fully explain the persistence and physiological resistance to weight change observed in many individuals. Buscemi et al. (October 15, 2025) published an open access review in Eating and Weight Disorders – Studies on Anorexia, Bulimia and Obesity proposing that obesity can be understood as a dysregulation of a central energy balance regulator called the ponderostat, a neuroendocrine set-point mechanism involving hypothalamic and higher brain circuits that integrates peripheral signals such as leptin, ghrelin and nutrient status to modulate hunger, satiety, energy expenditure and weight stability, a perspective that addresses gaps in prior research by framing obesity not just as a peripheral metabolic disorder but as a condition of disrupted central sensing and regulation.
This study demonstrates that obesity can be understood as a consequence of central dysregulation of the ponderostat, a neuroendocrine set-point mechanism that integrates signals from hypothalamic, cortical, and peripheral pathways to maintain energy balance. Dysregulation elevates the body-weight set-point in obese individuals, triggering compensatory hunger, reduced energy expenditure, and behavioral changes. These findings provide a mechanistic explanation for persistent weight gain and difficulty in sustaining weight loss, highlighting the need to target central regulatory systems, not just peripheral metabolism, for effective obesity interventions.
The ponderostat functions as a central control system, continuously integrating signals from hormones such as leptin, insulin, ghrelin, and nutrient availability, alongside neural inputs from the hypothalamus and higher brain regions. It regulates appetite, satiety, energy expenditure, and thermogenesis to maintain body weight within an individual-specific range. In obese individuals, dysregulation elevates the set-point, provoking compensatory increases in hunger, reductions in basal metabolic rate, and behavioral adaptations that resist weight loss. This central mechanism underscores obesity as a neuroendocrine disorder rather than solely a result of caloric imbalance.
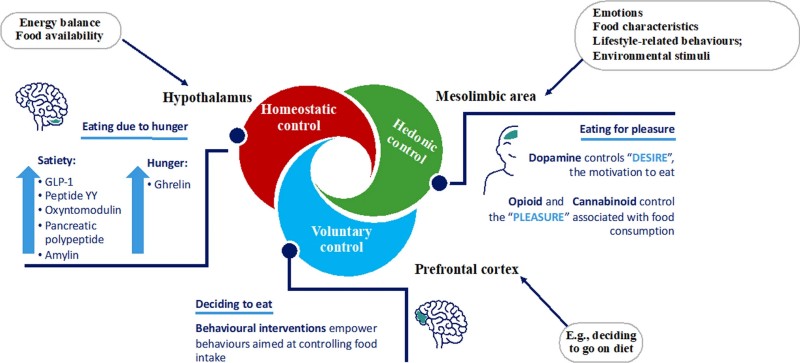 Fig.1 The brain regulates food intake through the ponderostat system. (Buscemi, et al., 2025)
Fig.1 The brain regulates food intake through the ponderostat system. (Buscemi, et al., 2025)
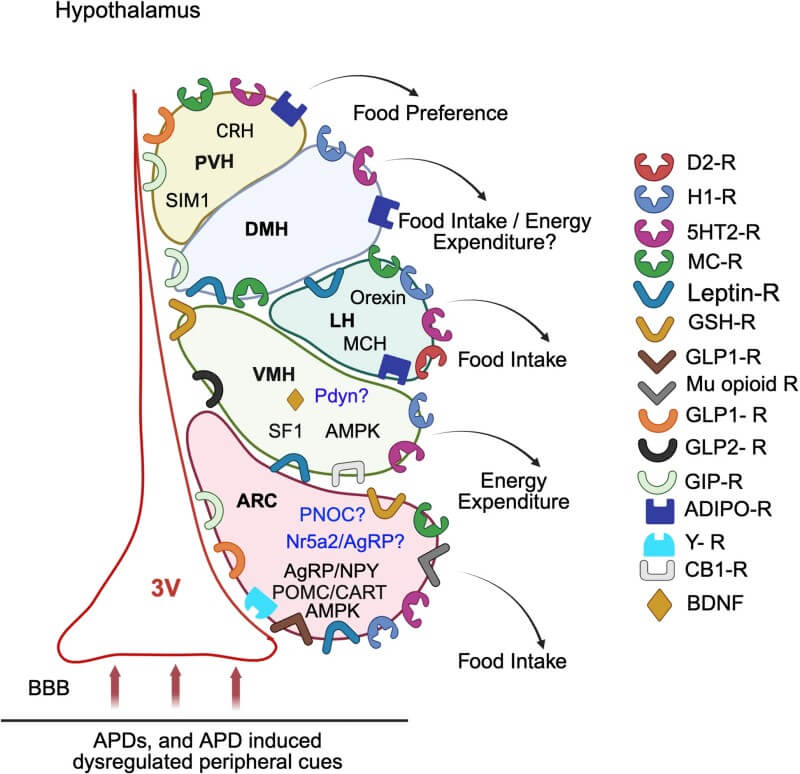
Obesity-related ponderostat dysregulation involves complex interactions among multiple brain regions. The hypothalamus processes homeostatic signals, the limbic system modulates reward-driven feeding, and the prefrontal cortex regulates executive control over eating behavior. Altered signaling among these regions amplifies appetite, increases hedonic responses to food, and reduces inhibitory control, collectively driving energy intake above expenditure. These neural alterations help explain why conventional interventions focusing on diet and exercise often fail to produce long-term weight loss and emphasize the need to target central regulatory pathways.
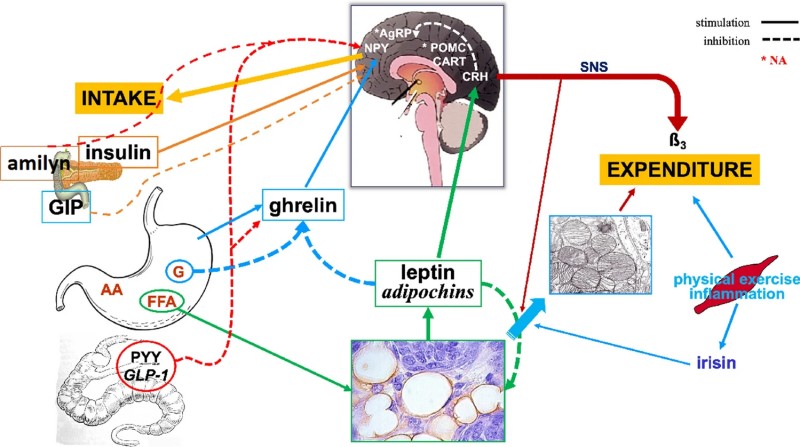 Fig.2 Neuroendocrine signals coordinate energy balance via the ponderostat. (Buscemi, et al., 2025)
Fig.2 Neuroendocrine signals coordinate energy balance via the ponderostat. (Buscemi, et al., 2025)
Prolonged deviations from the programmed body-weight set-point trigger powerful counter-regulatory mechanisms. These include increased appetite, heightened hedonic drive for high-calorie foods, decreased basal metabolic rate, and behavioral adaptations that restore weight toward the elevated set-point. Such compensatory responses explain the high rates of weight regain following calorie-restricted diets and highlight the resilience of the central regulatory system. Understanding these mechanisms is critical for designing interventions that not only reduce weight but also modulate central set-point regulation to achieve sustainable outcomes.
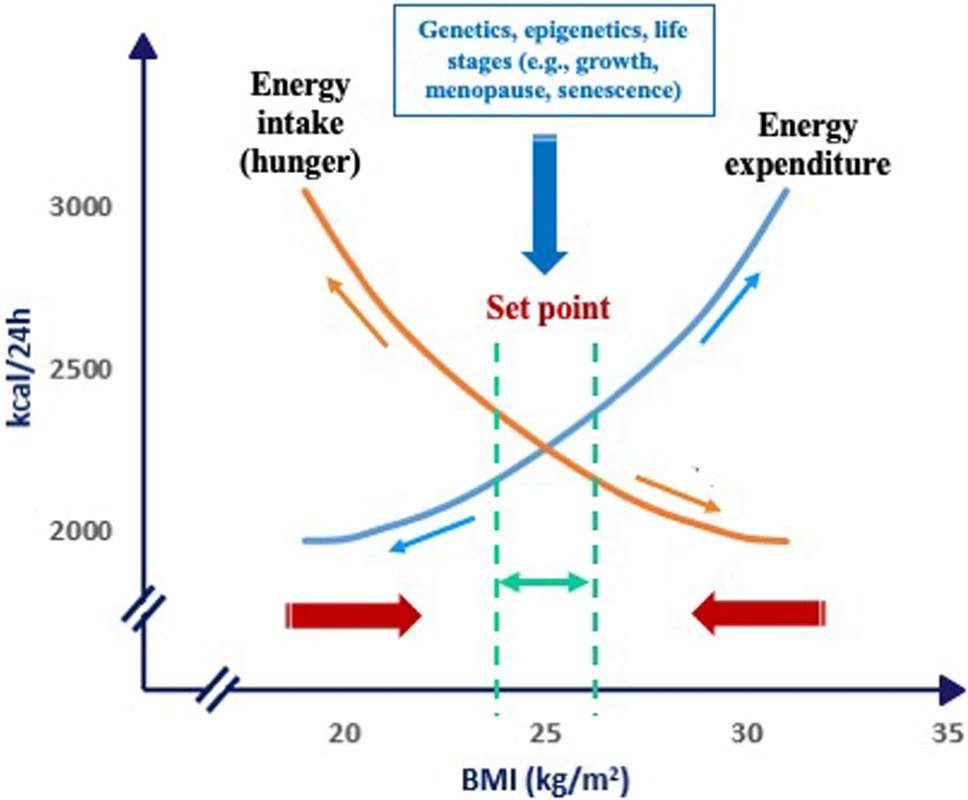 Fig.3 Body weight is maintained around a physiological set-point. (Buscemi, et al., 2025)
Fig.3 Body weight is maintained around a physiological set-point. (Buscemi, et al., 2025)
The ponderostat orchestrates a coordinated balance between energy intake and expenditure, integrating peripheral metabolic signals and central neural circuits to maintain stable body weight. Dysregulation shifts this balance toward chronic positive energy storage, resulting in sustained obesity. By framing obesity as a central regulatory disorder, this study underscores the importance of interventions targeting both central control mechanisms and peripheral metabolic pathways. Therapeutic strategies might include neuroendocrine modulators, behavioral interventions, and lifestyle modifications aimed at resetting the ponderostat to a healthier set-point.
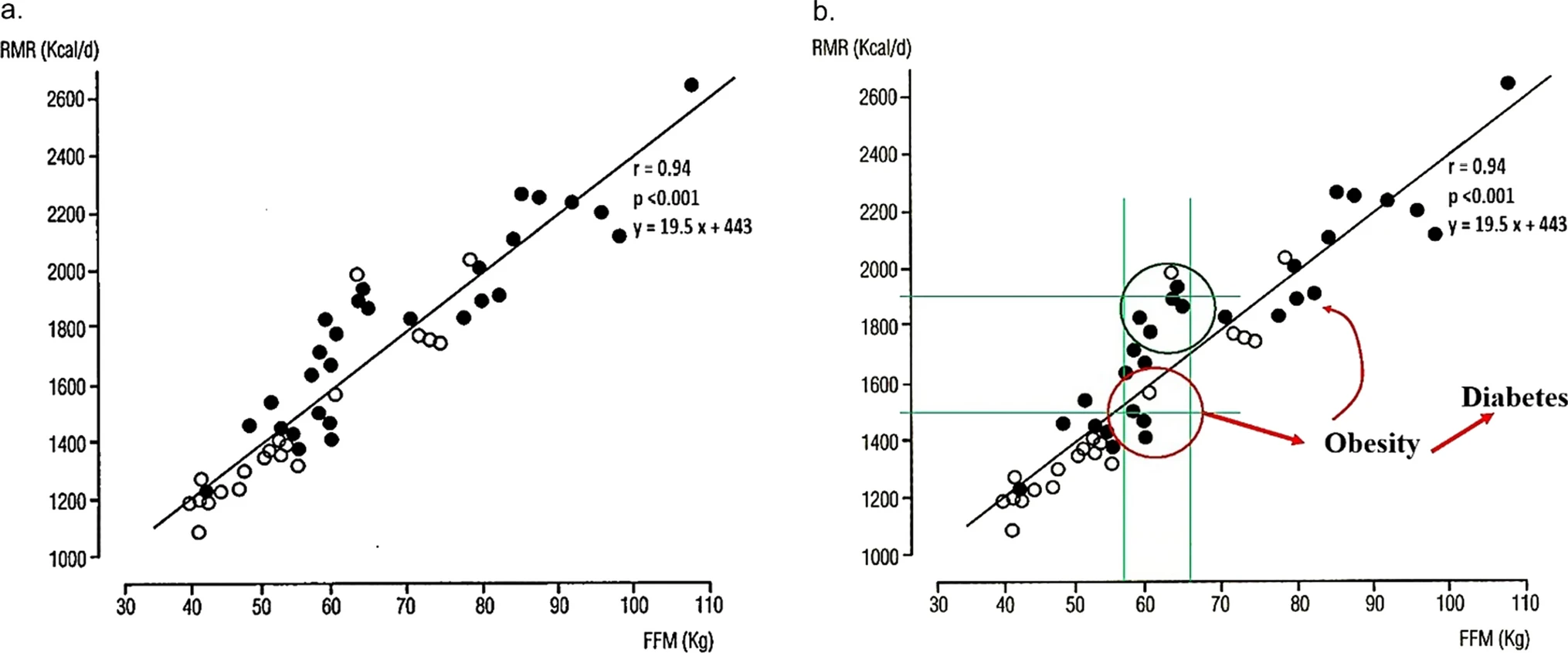 Fig.4 Individuals with lower RMR relative to FFM are more prone to obesity. (Buscemi, et al., 2025)
Fig.4 Individuals with lower RMR relative to FFM are more prone to obesity. (Buscemi, et al., 2025)
This perspective shifts the obesity paradigm toward understanding it as a central regulatory disorder wherein the neural system that senses and maintains body weight becomes dysregulated. Recognizing obesity as a condition of ponderostat dysfunction highlights why interventions focused solely on diet or exercise often fail to produce sustained weight loss: they do not correct the neuroendocrine set-point mechanisms that drive compensatory hunger and reduced energy expenditure. This framework suggests that effective obesity therapies may need to target central regulatory pathways, such as hypothalamic nutrient and hormone sensing, reward-related circuits, and cognitive control regions, potentially guiding development of combined neuromodulatory, pharmacologic, and behavioral interventions for durable metabolic balance.
For researchers investigating central energy balance regulation, hypothalamic signaling mechanisms, or neural set-point modulation in obesity, Protheragen offers Advanced Support, including central nervous system phenotyping, neuroendocrine pathway analysis, in vivo metabolic regulation studies, brain-behavior integration assays, and multi-omics data interpretation, enabling comprehensive exploration of central sensing and regulation in metabolic disease.
Reference
Copyright © Protheragen. All rights reserves.