- Home
- Microbiome and Microenvironment
- Gut Microbiome Differences in Obese and Non‑Obese Pregnant Women Insights from a Swedish Cohort
Gut Microbiome Differences in Obese and Non‑Obese Pregnant Women Insights from a Swedish Cohort
November 15, 2025
The gut microbiome plays a pivotal role in metabolism, energy balance, and inflammation, all of which are critical during pregnancy. Obesity in pregnant women is linked to higher risks of gestational diabetes, hypertension, and preeclampsia, but the underlying microbial mechanisms remain unclear.
Patavoukas et al. (2025) conducted a matched cohort study in Sweden, published in BMC Microbiology, to explore differences in the fecal microbiome between obese and non-obese pregnant women. While previous studies suggested associations between maternal obesity and gut dysbiosis, large, well-controlled cohort studies capturing temporal changes during gestation were lacking. This study addresses this gap by profiling the microbiome at two pregnancy time points in a robustly matched cohort.
Highlights
- Matched Cohort Design: 254 obese and 746 lean pregnant women matched for age and gestational week.
- Temporal Sampling: Fecal microbiome analyzed in the first and third trimesters, revealing dynamic changes over pregnancy.
- In-depth Microbiome Characterization: Detailed taxonomic resolution at the species scale, enabling the pinpointing of distinct microbial clusters tied to metabolic obesity.
- Focus on Metabolic Relevance: Functional predictions, including short-chain fatty acid (SCFA) production potential.
- Control of Confounders: Adjusted for bowel transit time and other physiological variables.
Key Findings
This study leveraged the large longitudinal Swedish SweMaMi cohort to characterize gut microbiome differences between 746 lean and 254 obese pregnant women at two pregnancy timepoints (second and early third trimester). The analyses included taxonomic diversity, beta diversity, differentially abundant species, and gut-metabolic modules (GMMs) based on shotgun metagenomic sequencing.
- Obesity Is Associated with Reduced Microbial Diversity and Richness
- Throughout the study duration, a marked reduction in microbial diversity was observed in pregnant participants with obesity relative to the lean cohort. Specifically, obese individuals exhibited persistent deficits in taxonomic richness, Shannon entropy, and Pielou's evenness. Quantitative gaps in observed richness remained significant at both intervals (TP1: 300.7 vs. 277.3; TP2: 308.5 vs. 282.5; p<0.0001), accompanied by a steady decline in both Shannon diversity (p<0.0003) and community evenness (p<0.05).
- A negative correlation between BMI and alpha diversity metrics was confirmed, indicating that higher BMI scores were associated with less species-rich and less even microbiomes.
- Although both lean and obese participants showed slight increases in observed species richness over time, statistically significant increases were only seen in the lean group, suggesting that pregnancy-associated diversification may be blunted in obesity.
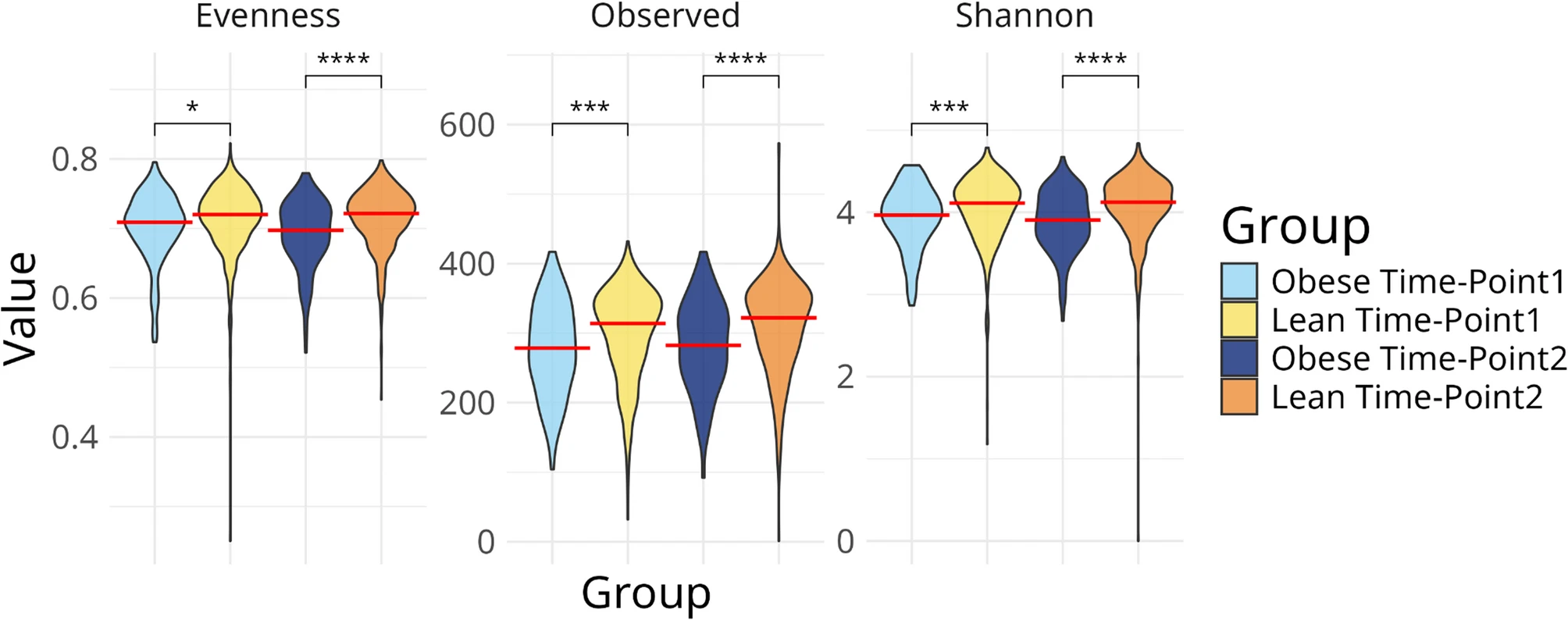 Fig.1 Obese pregnant women have lower gut microbiome diversity, richness, and evenness compared with lean women. (Patavoukas, et al., 2025)
Fig.1 Obese pregnant women have lower gut microbiome diversity, richness, and evenness compared with lean women. (Patavoukas, et al., 2025)
- Distinct Community Structure Between Obese and Lean Groups (Beta Diversity)
- Both presence/absence (Jaccard) and quantitative (Aitchison) distance metrics showed significant differences in community composition between obese and lean groups at both timepoints (p=0.001).
- Crucially, other host-specific and extrinsic variables, including intestinal transit speed, nutritional patterns, and the use of probiotic or antibiotic treatments, were identified as primary contributors to overall microbial divergence.
- When comparing within-subject changes over time, lean women exhibited more stable microbiome compositions (smaller intra-individual beta distances) than obese women, suggesting increased microbial fluctuation during pregnancy in the obese group.
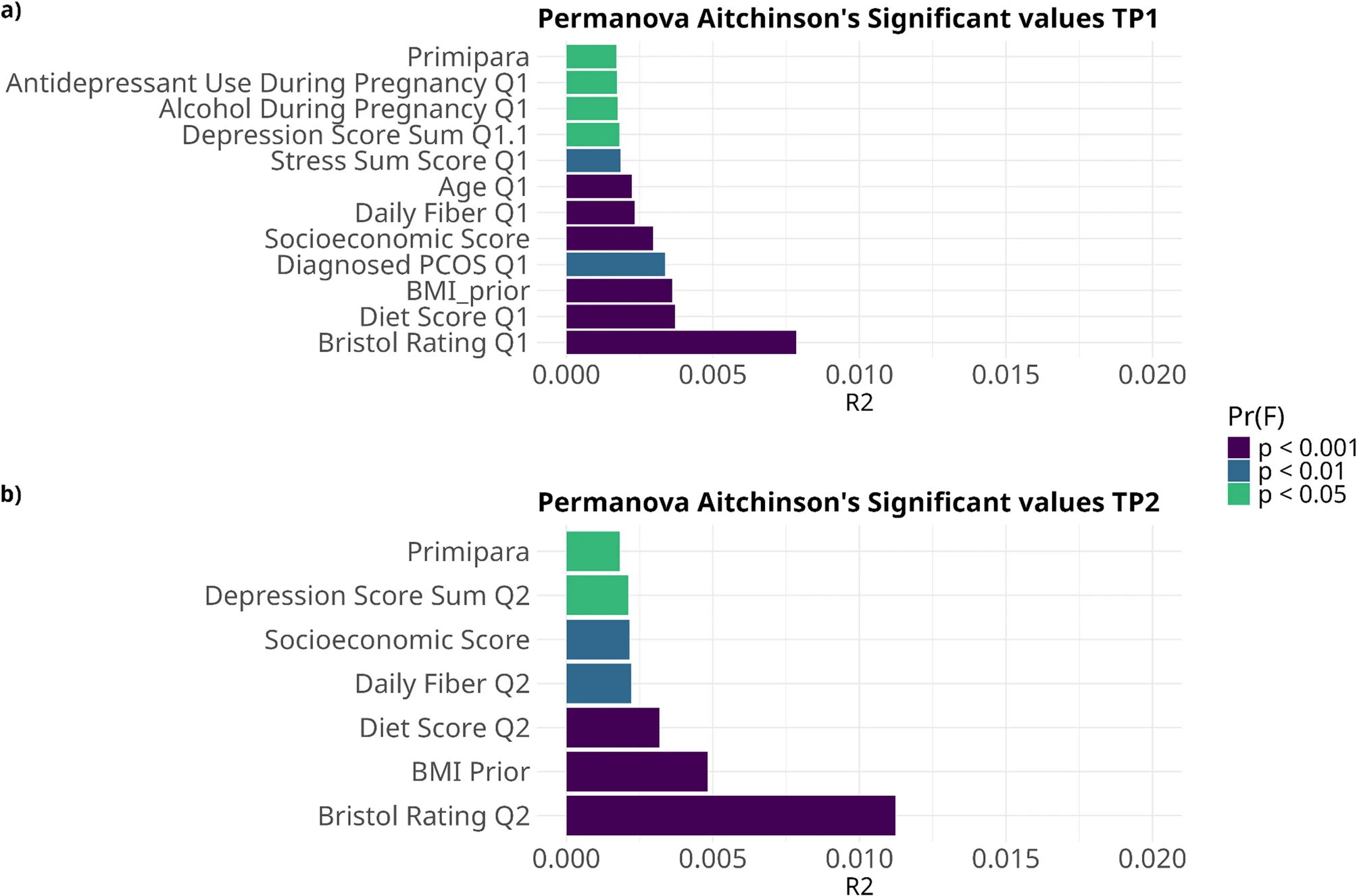 Fig.2 Stool form, BMI, antibiotics, and probiotics are major factors explaining microbiome differences between samples. (Patavoukas, et al., 2025)
Fig.2 Stool form, BMI, antibiotics, and probiotics are major factors explaining microbiome differences between samples. (Patavoukas, et al., 2025)
- Differential Species Abundance Reveals Taxonomic Shifts
Adjusted analyses showed that maternal obesity is associated with distinct taxonomic shifts over pregnancy. In the second trimester, a few species were differentially enriched between obese and lean women, expanding by the third trimester, although controlling for bowel transit reduced most differences. Notably, obese women exhibited higher abundances of opportunistic pathogens and taxa linked to inflammation and metabolic dysregulation, including Streptococcus mitis, S. parasanguinis, and Collinsella aerofaciens. Certain Firmicutes also differed between groups, reflecting diet-associated microbiome signatures. These results highlight specific microbial patterns accompanying maternal obesity, beyond overall reductions in diversity.
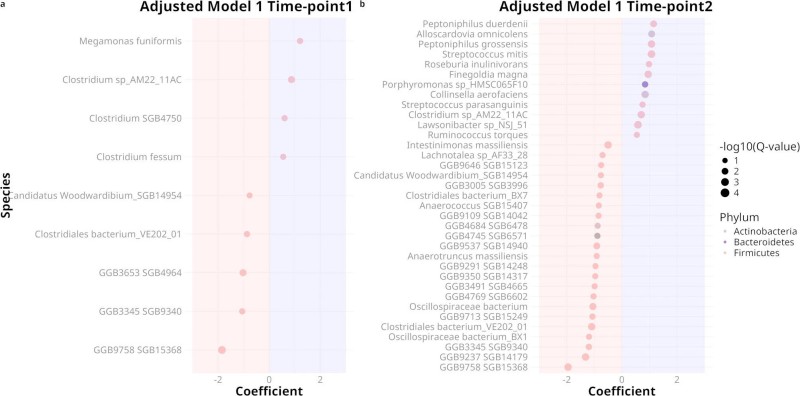 Fig.3 Several Firmicutes species differ in abundance between obese and lean pregnant women across pregnancy. (Patavoukas, et al., 2025)
Fig.3 Several Firmicutes species differ in abundance between obese and lean pregnant women across pregnancy. (Patavoukas, et al., 2025)
- Functional Alterations: Gut Metabolic Modules (GMMs)
Functional profiling of the microbiome using KEGG-based gut metabolic modules revealed:
- Multiple GMMs were differentially abundant between lean and obese groups in early pregnancy under adjusted models, but this pattern weakened in late pregnancy.
- Propionate production capacity was consistently higher in lean individuals across 4 out of 6 statistical models, even after controlling for transit time and other confounders.
Propionate is a microbial-derived short-chain fatty acid known to mediate anti-inflammatory responses, enhance insulin sensitivity, and regulate adipose tissue turnover during pregnancy. Consequently, the sustained reduction of this metabolite in the microbiomes of obese women likely represents a functional deficiency associated with increased metabolic vulnerability.
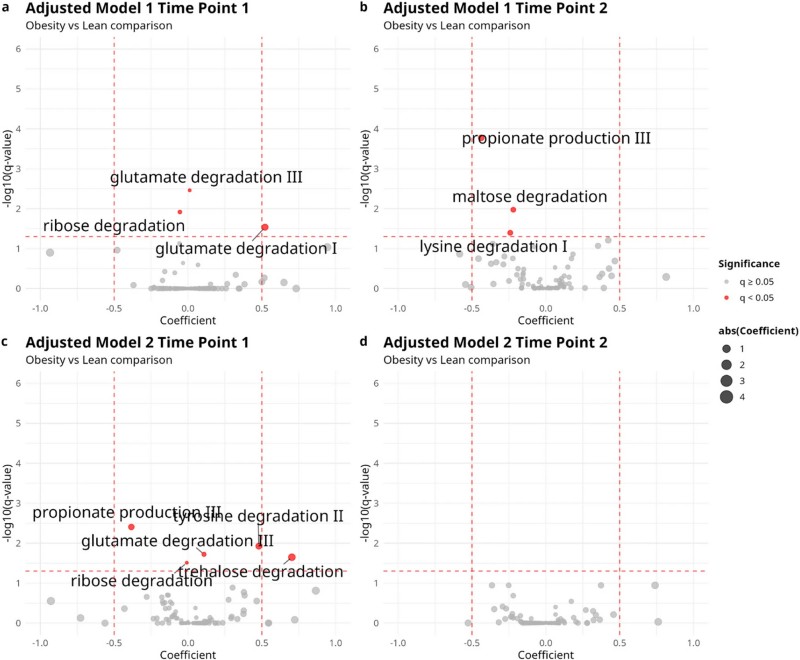 Fig.4 Functional gut metabolic modules differ between obese and lean women. (Patavoukas, et al., 2025)
Fig.4 Functional gut metabolic modules differ between obese and lean women. (Patavoukas, et al., 2025)
Interpretation & Translational Value
This study highlights that maternal obesity is associated with altered gut microbiome composition and functional potential, which may influence metabolic and inflammatory processes during pregnancy. In particular, the observed reduction in short-chain fatty acid (SCFA) production suggests a microbial contribution to impaired glucose metabolism and heightened inflammation in obese pregnancies.
Understanding these microbiome dynamics carries important relevance, as it may guide strategies to reduce obesity-related pregnancy complications. Interventions such as dietary modulation, probiotics, or synbiotics could be investigated to normalize maternal gut microbiota and improve metabolic outcomes.
Research Support
For researchers interested in exploring microbiome dynamics, gut microbiome interventions, or metabolic studies, Protheragen offers Comprehensive Research Services to support experimental design, microbiome profiling, and data analysis.
| Obesity Microbiota Colonization Studies |  |
Advanced Gut Microbiota Profiling in Obesity |
| Genetics Analysis Service of Microbiota in Obesity | Effect Analysis of Dietary Components on the Gut Microbiota | |
| Obesity Microbiota Metabolite Testing Service | Fecal Microbiota Transplantation Research Service | Obesity Gut microbiota-targeted intervention Service |
Reference
- Patavoukas, E.; et al. Differences in the faecal microbiome of obese and non-obese pregnant women: a matched cohort study in Sweden. BMC Microbiol. 2025, 25(1): 750. (CC BY 4.0)